 Frozen shoulder, or adhesive capsulitis, is a condition that begins with a gradual onset of pain and a limitation of shoulder motion. The discomfort and loss of movement can become so severe that even simple daily activities become difficult. Although much is known about this condition, there continues to be considerable controversy about its causes and the best ways to treat it.
Frozen shoulder, or adhesive capsulitis, is a condition that begins with a gradual onset of pain and a limitation of shoulder motion. The discomfort and loss of movement can become so severe that even simple daily activities become difficult. Although much is known about this condition, there continues to be considerable controversy about its causes and the best ways to treat it.
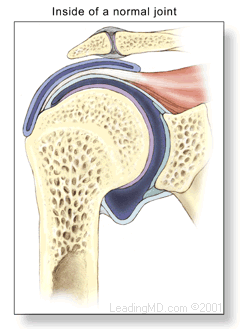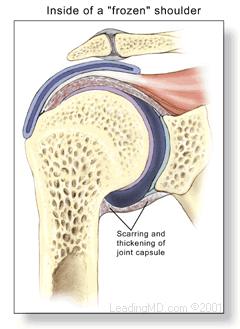
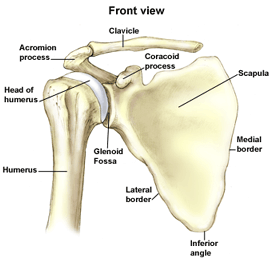
The shoulder is the most mobile joint in the human body, with a complex arrangement of structures working together to provide the movement necessary for daily life. Unfortunately, this great mobility comes at the expense of stability. Several bones and a network of soft tissue structures (ligaments, tendons, and muscles), work together to produce shoulder movement. They interact to keep the joint in place while it moves through extreme ranges of motion. Each of these structures makes an important contribution to shoulder movement and stability. Certain work or sports activities can put great demands upon the shoulder, and injury can occur when the limits of movement are exceeded and/or the individual structures are overloaded.
What is frozen shoulder?
Frozen shoulder, also called adhesive capsulitis, is a thickening and tightening of the soft tissue capsule that surrounds the glenohumeral joint, the ball and socket joint of the shoulder. When the capsule becomes inflamed, scarring occurs and adhesions are formed. This scar formation greatly intrudes upon the space needed for movement inside the joint. Pain and severely limited motion often occur as the result of the tightening of capsular tissue.
There are two types of frozen shoulder: primary adhesive capsulitis and secondary adhesive capsulitis.
- Primary adhesive capsulitis is a subject of much debate. The specific causes of this condition are not yet known. Possible causes include changes in the immune system, or biochemical and hormonal imbalances. Diseases such as diabetes mellitus, and some cardiovascular and neurological disorders may also be contributing factors. In fact, patients with diabetes have a three times higher risk of developing adhesive capsulitis than the general population. Primary adhesive capsulitis may affect both shoulders (although this may not happen at the same time) and may be resistant to most forms of treatment.
- Secondary (or acquired) adhesive capsulitis develops from a known cause, such as stiffness following a shoulder injury, surgery, or a prolonged period of immobilization.
With no treatment, the condition tends to last from one to three years. Many patients are unwilling to endure the pain and limitations of this problem while waiting for it to run its natural course. Even after many years, some patients will continue to have some stiffness, but no serious pain or functional limitations.
The major symptoms of frozen shoulder are pain and loss of motion
- - The onset of symptoms may be gradual or sudden, depending on the cause of the condition. With primary adhesive capsulitis, the onset of symptoms is usually gradual. A sudden onset of symptoms may follow an injury to the shoulder.
- - The pain and loss of function associated with this condition can become so severe that it can significantly affect the quality of life, and prevent some patients from sleeping well or working.
How is frozen shoulder diagnosed?
The diagnosis of frozen shoulder is made only after a careful history and physical examination is performed. Pain and loss of motion can be symptoms of many shoulder conditions, so a detailed assessment of the shoulder's full range of motion is important. A history of surgery or injury, or the presence of illnesses such as diabetes, is information the physician needs in order to make the correct diagnosis.
It is important to recognize the different patterns of motion loss. Primary adhesive capsulitis is usually associated with loss of motion in all directions. Secondary adhesive capsulitis more often has more defined loss of motion; affecting some movements, but not others.
In most cases, the history and examination are sufficient to determine the presence or absence of frozen shoulder. Imaging may occasionally be necessary to confirm the diagnosis and to identify other underlying problems.
- X-rays cannot reveal the cause of shoulder stiffness in most cases of primary adhesive capsulitis. However, in secondary adhesive capsulitis, X-rays can show signs of arthritis, fractures, or metallic plates that may be contributing to motion loss.
- An MRI (Magnetic Resonance Image) shows soft tissue and may be used in cases in which another disorder is suspected, such as a rotator cuff tear.
- An arthrogram may be used with an MRI to provide further information about structures in the shoulder. A dye is injected into the shoulder and images are obtained. The dye creates a contrast on the image, making the specific location of adhesions and the reduced space typical of frozen shoulder more visible.
How is frozen shoulder treated?
Non-Operative Treatment
For most patients with primary adhesive capsulitis, a supervised physical therapy program can help restore lost motion, although it can take six to eighteen months to accomplish this. It is often necessary to combine a home program with supervised physical therapy for maximum gains.
Shoulder stiffness that results from secondary adhesive capsulitis is generally more resistant to non-operative treatment. A supervised physical therapy program is always tried first. However, even an aggressive stretching program with an experienced therapist is often ineffective when frozen shoulder follows an injury or previous surgery.
In some cases, non-steroidal anti-inflammatory medications can be helpful with this condition. Other treatments such as ice, heat, and ultrasound may help alleviate some of the pain. These treatments are recommended as long as they are effective.
Supervised tor home herapy programs continues as long as the patient is making improvement. If the patient is not improving operative treatment may be considered. The expected time for resolution of frozen shoulder varies depending on the underlying causes and from patient to patient. The decision to undergo surgical treatment is made on a case by case basis depending on many factors. These include the cause of the frozen shoulder, the duration of treatment and underlying medical conditions.
Operative Treatment
Operative procedures to treat frozen shoulder include closed manipulation, as well as arthroscopic and open surgical techniques. Operative treatment of primary adhesive capsulitis should only be considered once severe pain has subsided, and discomfort is present only at the extremes of motion. Severe pain represents the inflammatory stage of the disease. Surgery during this inflammatory phase may actually increase injury to the joint capsule, adding to the patient’s loss of motion. Arthroscopic release of the contracted shoulder tissue is preferred by your physician as opposed to closed manipulation of the shoulder. This is because arthroscopic release is more precise and typically restores better motion than simply tearing the contracted tissues with a closed manipulation.
Most patients who have not done well with a non-operative therapy program will do well with a closed manipulation or an arthroscopic capsular release procedure that is followed by aggressive motion therapy.
Arthroscopic Capsular Release
Arthroscopic capsular release has proven to be a safe, effective way to release the scar tissue from the capsule. During an arthroscopy, a small fiberoptic instrument is inserted into the joint. The scar tissue surrounding the joint is removed and a gentle manipulation follows. This will significantly reduce the risk of fracture or injury if the frozen shoulder has been present for some time. If necessary, other disorders within the shoulder can be addressed at the same time.
Open Release
On rare occasions, an open procedure to release the adhesions may be required. This may be the case if tightening is present between tissues outside the joint capsule that are not accessible with arthroscopy. Patients who have had previous surgery or a severe joint injury are often candidates for an open release.
What types of complications may occur?
Complications after frozen shoulder surgery are generally infrequent. The most common problems associated with any of these procedures result from too little release, which fails to adequately reduce stiffness, or (very rarely) from too much release, which may cause shoulder instability. Fractures of the humerus have been reported with closed manipulation. Older patients with fragile bones (osteoporosis) are more at risk for this type of complication. In rare cases, previous surgical repairs have been damaged. Although arthroscopic releases are relatively safe, releases in certain areas inside the joint have led to nerve injury.
The recovery from non-operative treatment of frozen shoulder can take one to three years. It is important for patients with frozen shoulder to understand the natural course of the disease and how long it can persist. A home stretching program, combined with a supervised program with a skilled therapist, can speed the recovery process in many cases.
Operative
Following surgery:
- Patients usually remain in the hospital for one to two days. During this time, pain medication is delivered directly to the joint through a catheter.
- While in the hospital, patients begin an aggressive shoulder motion program supervised by a physical therapist.
- Patients are encouraged to use the treated arm for daily activities. A sling is not worn.
- Patients are put on a home stretching program that is to be done between structured therapy appointments.
- Surgical incisions are to be kept clean, dry, and covered until the doctor sees the patient at the follow-up visit, normally about ten days after surgery. Stitches are usually removed at this time.
- Progress is closely monitored with regular office visits. Specific weaknesses or motion limitations are addressed during these visits.
- The strengthening phase of a rehabilitation program begins after the patient has achieved a full, pain-free arc of motion. This generally takes at least three months.
FAQs
1. Why did I develop a frozen shoulder?
We do not have a good explanation for the development of frozen shoulder in most patients.
The majority of cases seem to be more prevalent in women, diabetics, and those with hypothyroidism. Others who develop frozen shoulder are those who have sustained an injury and developed stiffness as a result. The trauma can be quite mild or severe, and the body’s response to the event is probably more important than the event itself.
2. How can frozen shoulder be treated?
The resolution of a frozen shoulder can be very slow, but physical therapy can speed up the healing process. Frozen shoulder begins with pain followed by the rapid development of stiffness. Usually when the pain starts to subside physical therapy can be effective in stretching the capsule back out. Occasionally in unmanageable cases surgery is indicated. This is true only in cases in which the pain has subsided and the residual capsular contracture has not responded to six months or more of physical therapy. Early surgery in the face of frozen shoulder will lead to more problems with stiffness after surgery.
3. I have been diagnosed with a rotator cuff tear in addition to frozen shoulder; why won’t the surgeon repair the rotator cuff now?
Surgery in the face of a frozen shoulder is not recommended because of the immobilization required after a rotator cuff repair. The shoulder becomes more inflamed after the surgery and the immobilization required to heal the cuff repair leads to increased stiffness. The only way to deal with this combination of problems is to allow physical therapy to stretch out the frozen shoulder. Once that has been accomplished, the rotator cuff repair can be performed. The shoulder will probably be stiffer than the average cuff repair after the immobilization period ends, but research has shown that physical therapy can help regain lost motion.